




Lupus Manifestations
Medicine, surgery,ophthalmology,psychiatry,dermatology,ENT disease,treatment,cure,diagnosis,complications, Medical cases Ebooks free downloads medical videos Gallery



| Measles | | Number 10 |
| Polio | | Number 9 |
| Yellow Fever | | Number 8 |
| AIDS | | Number 7 |
| Malaria | | Number 6 |
| Tuberculosis (TB) | | Number 5 |
| Cholera | | Number 4 |
| Plague (bubonic and Pneumonic) | | Number 3 |
| Smallpox | | Number 2 |
| Influenza or “flu” | | Number 1 |
 s
sMyasthenia gravis (literally "serious muscle-weakness") is a neuromuscular disease leading to fluctuating muscle weakness and fatiguability. It is an autoimmune disorder, in which weakness is caused by circulating antibodies that block acetylcholine receptors at the post-synaptic neuromuscular junction, inhibiting the stimulative effect of the neurotransmitter acetylcholine. Myasthenia is treated medically with cholinesterase inhibitors or immunosuppressants, and, in selected cases, thymectomy. At 200–400 cases per million it is one of the less common autoimmune disorders.
Signs and symptoms
The hallmark of myasthenia gravis is fatiguability. Muscles become progressively weaker during periods of activity and improve after periods of rest. Muscles that control eye and eyelid movement, facial expression, chewing, talking, and swallowing are especially susceptible. The muscles that control breathing and neck and limb movements can also be affected. Often the physical examination is within normal limits.[3]
The onset of the disorder can be sudden. Often symptoms are intermittent. The diagnosis of myasthenia gravis may be delayed if the symptoms are subtle or variable.
In most cases, the first noticeable symptom is weakness of the eye muscles. In others, difficulty in swallowing and slurred speech may be the first signs. The degree of muscle weakness involved in MG varies greatly among patients, ranging from a localized form, limited to eye muscles (ocular myasthenia), to a severe or generalized form in which many muscles - sometimes including those that control breathing - are affected. Symptoms, which vary in type and severity, may include asymmetrical ptosis (a drooping of one or both eyelids), diplopia (double vision) due to weakness of the muscles that control eye movements, unstable or waddling gait, weakness in arms, hands, fingers, legs, and neck, a change in facial expression, dysphagia (difficulty in swallowing), shortness of breath and dysarthria (impaired speech, often nasal due to weakness of the velar muscles).
In myasthenic crisis a paralysis of the respiratory muscles occurs, necessitating assisted ventilation to sustain life. In patients whose respiratory muscles are already weak, crises may be triggered by infection, fever, an adverse reaction to medication, or emotional stress.[4] Since the heart muscle is stimulated differently, it is never affected by MG.
DiagnosisMyasthenia can be a difficult diagnosis, as the symptoms can be subtle and hard to distinguish from both normal variants and other neurological disorders. A thorough physical examination can reveal easy fatiguability, with the weakness improving after rest and worsening again on repeat of the exertion testing. Applying ice to weak muscle groups characteristically leads to improvement in strength of those muscles. Additional tests are often performed, as mentioned below. Furthermore, a good response to medication can also be considered a sign of autoimmune pathology.
Muscle fatigability can be tested for many muscles.A thorough investigation includes:
If the diagnosis is suspected, serology can be performed in a blood test to identify certain antibodies:

A chest X-ray is frequently performed; it may point towards alternative diagnoses (e.g. Lambert-Eaton due to a lung tumor) and comorbidity. It may also identify widening of the mediastinum suggestive of thymoma, but computed tomography (CT) or magnetic resonance imaging (MRI) are more sensitive ways to identify thymomas, and are generally done for this reason.
Myasthenia Gravis is associated with various autoimmune diseases, including:
Contact dermatitis is a localized rash or irritation of the skin caused by contact with a foreign substance. Only the superficial regions of the skin are affected in contact dermatitis. Inflammation of the affected tissue is present in the epidermis (the outermost layer of skin) and the outer dermis (the layer beneath the epidermis).Unlike contact urticaria, in which a rash appears within minutes of exposure and fades a
way within minutes to hours, contact dermatitis takes days to fade away. Even then, contact dermatitis fades only if the skin no longer comes in contact with the allergen or irritant. Contact dermatitis results in large, burning, and itchy rashes, and these can take anywhere from several days to weeks to heal. Chronic contact dermatitis can develop when the removal of the offending agent no longer provides expected relief.
In North/South America, the most common causes of allerg ic contact dermatitis are plants of the Toxicodendron genus: poison ivy, poison oak, and poison sumac. Specific plant species that can induce
ic contact dermatitis are plants of the Toxicodendron genus: poison ivy, poison oak, and poison sumac. Specific plant species that can induce

such contact dermatitis include Western Poison Oak, a widespread plant in the western USA. Common causes of irritant contact dermatitis are harsh (highly alkaline) soaps, detergents, and cleaning products.
There are three types of contact dermatitis: irritant contact, allergic contact, and photocontact dermatitis. Photocontact dermatitis is divided into two categories: phototoxic and photoallergic.
Plants
Allergic contact dermatitisSometimes termed "photoaggravated"(Bourke et al. 2001)[17], and divided into two categories, phototoxic and photoallergic, PCD is the eczematous condition which is triggered by an interaction between an otherwise unharmful or less harmful substance on the skin and ultraviolet light (320-400 nm UVA) (ESCD 2006), therefore manifesting itself only in regions where the sufferer has been exposed to such rays. Without the presence of these rays, the photosensitiser is not harmful. For this reason, this form of contact dermatitis is usually associated only with areas of skin which are left uncovered by clothing. The mechanism of action varies from toxin to toxin, but is usually due to the production of a photoproduct. Toxins which are associated with PCD include the psoralens. Psoralens are in fact used therapeutically for the treatment of psoriasis, eczema and vitiligo.
Photocontact dermatitis is another condition where the distinction between forms of contact dermatitis is not clear cut. Immunological mechanisms can also play a part, causing a response similar to ACD.
Allergic dermatitis is usually confined to the area where the trigger actually touched the skin, whereas irritant dermatitis may be more widespread on the skin. Symptoms of both forms include the following:
While either form of contact dermatitis can affect any part of the body, irritant contact dermatitis often affects the hands, which have been exposed by resting in or dipping into a container (sink, pail, tub, Sun, Swimming Pools With High chlorine ), containing the irritant.
- Weak acid solutions [lemon juice, vinegar] can be used to counteract the effects of dermatitis contracted by exposure to basic irritants [phenol etc.].
If the rash does not improve or continues to spread after 2-3 of days of self-care, or if the itching and/or pain is severe, the patient should contact a dermatologist or other physician or physician assistant. Medical treatment usually consists of lotions, creams, or oral medications.
Since contact dermatitis relies on an irritant or an allergen to initiate the reaction, it is important for the patient to identify the responsible agent and avoid it. This can be accomplished by having patch tests, a method commonly known as allergy testing. The patient must know where the irritant or allergen is found to be able to avoid it. It is important to also note that chemicals sometimes have several different names.[18]
In an industrial setting the employer has a duty of care to the individual worker to provide the correct level of safety equipment to mitigate the exposure to harmful irritants. This can take the form of protective clothing, gloves or barrier cream depending on the working environment.

Reprinted from Times Magazine, By Christine Gorman
Spring 1988The year was 1959, location: The central African city of Leopoldville, now called Kinshasa, shortly before the waves of violent rebellion that  followed the liberation of the Belgian Congo. A seemingly healthy man walked into a hospital clinic to give blood for a Western backed study of blood diseases. He walked away and was never heard from again. Doctors analyzed his sample, froze it in a test tube and forgot about it. A quarter-century later, in the mid-1980s, researchers studying the growing AIDS epidemic took a second look at the blood and discovered that it contained HIV, the virus that causes AIDS.
followed the liberation of the Belgian Congo. A seemingly healthy man walked into a hospital clinic to give blood for a Western backed study of blood diseases. He walked away and was never heard from again. Doctors analyzed his sample, froze it in a test tube and forgot about it. A quarter-century later, in the mid-1980s, researchers studying the growing AIDS epidemic took a second look at the blood and discovered that it contained HIV, the virus that causes AIDS.
And not just any HIV. The Leopoldville sample is the oldest specimen of the AIDS virus ever isolated and may now help solve the mystery of how and when the virus made the leap from animals (monkeys or chimpanzees) to humans, according to a report published last week in Nature. Dr. David Ho, director of the Aaron Diamond AIDS Research Center in New York City and one of the study's authors, says a careful genetic analysis of the sample's DNA pushes the origin of the AIDS epidemic back at least a decade, to the early '50s or even the '40s.
Over the past 15 years, scientists have identified at least 10 subtypes of the virus. But they couldn't tell whether they were seeing variations on one changeable virus or the handiwork of several different viruses that had made the jump from primates to man. A look at the genetic mutations in the Leopoldville sample strongly suggests that all it took to launch the epidemic was one unlucky turn of events.
The findings underscore how rapidly HIV can adapt to its surroundings, making it difficult to develop effective vaccines. No one knows how many more subtypes of HIV will sprout in the next 40 years, but chances are they will be every bit as lethal as the ones we see today, if not more so.
 Apert Syndrome
Apert Syndrome

Apert syndrome is a rare genetic disorder that is characterized by specific craniofacial and limb abnormalities. It is caused by a genetic mutation in the FGFR2 gene on chromosome 10. The mutation can be inherited from a parent who has Apert syndrome or it can be a spontaneous (new) mutation. Studies show that Apert syndrome tends to occur more often in children with older fathers. Furthermore, all new mutations (those that have not been inherited by an affected parent) have been shown to occur exclusively in the FGFR2 gene received by the father. Apert syndrome occurs in 1 out of 100,000 to 160,000 live births and affects males and females equally. The first reported case of the syndrome was in 1848 by S.W. Wheaton, and in 1906, a French physician named E. Apert described nine cases and defined the syndrome.
Features and Characteristics
The following characteristics have been found in children with Apert syndrome:
| Hyperhidrosis Synonychia Brittle nails Severe acne in puberty Interruption of the eyebrows Hypopigmentation Hyperkeratosis Paronychial infections of plantar skin Excessive skin wrinkling of forehead Dimples at knuckles, shoulders and elbows |
Prematurely Fused Cranial Sutures
Retruded Mid-face
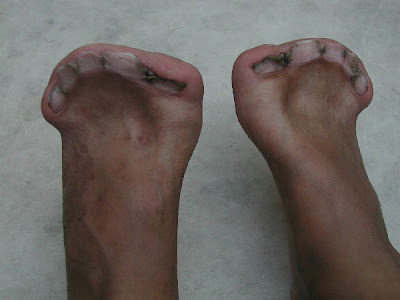
Fused Fingers and Toes
Diagnosis
The diagnosis can be made by a skull x-ray, which will confirm premature closure of the skull, and by a clinical exam. The combination of the craniofacial problems and the fused fingers and toes is what distinguishes Apert syndrome from other similar syndromes. Since the defect which causes Apert syndrome has been identified, genetic testing can be provided to confirm a diagnosis.
Treatment
Treating a child with Apert syndrome is best accomplished with a team approach. This would include a craniofacial surgeon, neurosurgeon, ENT specialist, audiologist, speech pathologist, oral surgeon, psychologist, ophthalmologist, and an orthodontist. The majority of treatment methods is surgical and the individual will likely require many operations. Aside from the surgeries required to correct the craniofacial problems and the fused fingers and toes, there may be other potential surgeries to improve the upper airway, address severe eye problems, or correct dental issues.